“When he shall die, take him and cut him out in little stars, and he will make the face of heaven so fine that all the world will be in love with night and pay no worship to the garish sun.” – William Shakespeare.
Susan was moved to a private room this morning. I noticed when I came in that the tubes and machines had been removed or disconnected. I saw she was in what hospitals call comfort care. The doctors can’t treat what can’t be treated.
Susan asked me, as Ed Gulley did, to write truthfully and openly about her sickness and fate. So I am trying. Like many people at the edge of life, she wants to be seen and known, especially at this difficult time.
She says, as Ed did, that her death may give some meaning to her life.
Susan has lived difficult and often painful life, if I were to hope and pray for anything, it would be for her to find some peace. Susan was always talking about taking care of herself, losing weight, walking more, changing her diet, exercising, altering her “lifestyle.” She needn’t worry about that anymore.
I told her she can just be Susan.
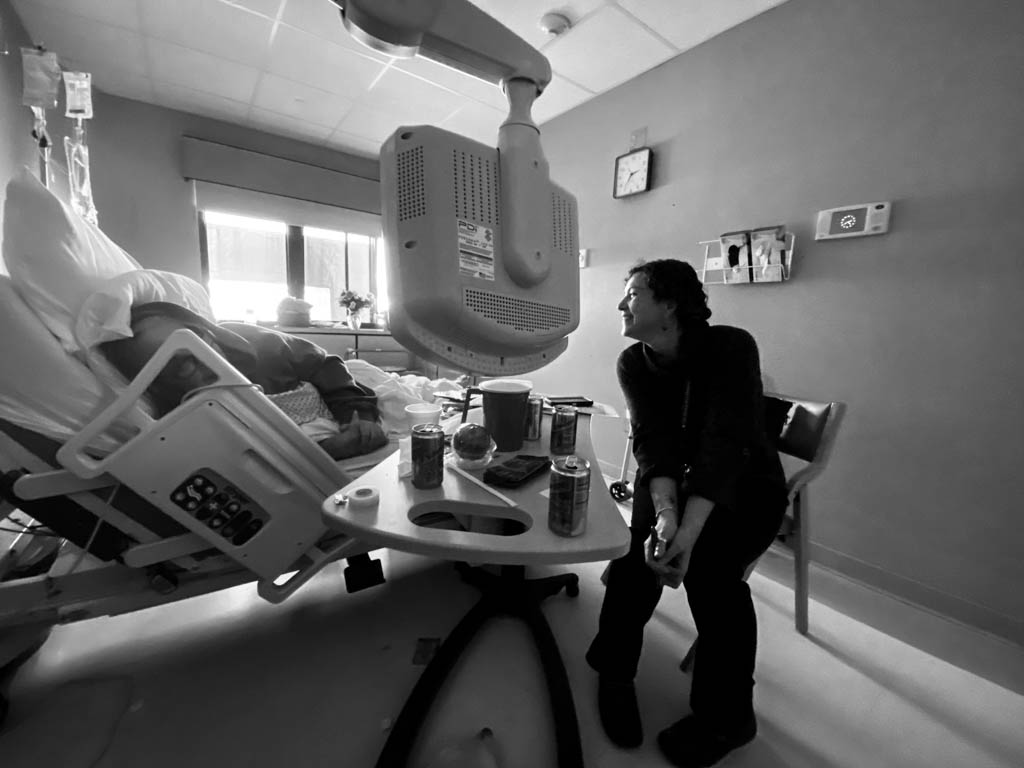
Her brother returned to California today, her friend Donna is in New Jersey caring for her mother. I met with a member of the Palliative Care Team and also Kate (above) from hospice in her room.
It was difficult for her to stay awake, even as her life was discussed. It is a powerful thing to witness her decline each day.
We were there, after all the tests and diagnoses, to find out what’s next for Susan.
And we know now. A member of the medical team leaned forward and told Susan what I think we both already suspected: “you will almost certainly pass away in this room.” There is nothing more they can do.
Susan was lucid at times, incoherent at others. Like many liver patients, she was sleeping on and off, even throughout the meeting. She wanted to know if she would be able to sightsee or travel, and she was told no, that would almost certainly be impossible.
Kate patiently and lovingly answered each of her questions, sometimes more than once.
Donna and I both agreed that Sally shouldn’t come to the hospital for a farewell visit to Susan.
She is adapting wonderfully to her foster home, and we all think a visit could be disruptive and confusing to the dog, who has been through enough.
Sally’s ultimate home is not yet certain. She might remain where she is, or go to Portland, Oregon, or another home in New Jersey. All are very good options.
I told Susan I believe it’s time for Sally to go on living her life, she is happy and loved.
This is up to Donna Nicosia, Susan’s best and most trusted friend. Donna is coming to Saratoga Tuesday to say goodbye to her friend.
There is more work to be done to ensure Susan gets the care she needs.
Switching to hospice is a complex administrative, medical, and insurance issue; it can’t be done instantly or simply in Susan’s case. Nothing is straightforward when it comes to health care, and the insurance company is the most powerful player.
Hospice is now involved, as we hoped. Susan agreed. I tried to arrange a will for Susan, but she was not lucid enough to do that today. I spoke with her brother about funeral arrangements, that was a hard conversation for him.
Hospice has begun working with the hospital, going over medications and tests and treatment to eliminate what can be eliminated, and to make Susan as comfortable as possible. I was happy to see them there, I know and trust Susan will be comfortable now. I can take a deep breath.
This is the final phase of her journey; she understands this and accepts it.
She does not feel defeated, somewhat resigned. “What can I do?” she kept saying. She joked with me a few times, and told Kate that I could be testy at times. I did get her to laugh. Zinnia got her to smile.
But there wasn’t much for her to laugh about today. She is digesting what is happening to her, no longer ducking it or avoiding it.
She knows she is dying, and soon.
There was something surreal about this, yet also liberating and peaceful. Susan can now get on with the formidable task of figuring out how to spend the rest of her time in this world.
She no longer needs to worry about what the tests will show or the doctors will find.
With her brother gone, there are no family here, no grieving spouse or children, nieces and nephews, parents, or grandparents. Susan has few friends, but they love her very much.
Donna and I are her family now, something I know I did not anticipate. Donna has been family for a while.
But we take this responsibility seriously and talk to one another often. We will be there for her. I am glad to be in a position to help.
The mission has shifted from gathering information to making sure she is comfortable. It is simpler really, the hospital and hospice will do the hard part.
I will have to go back to the hospital this weekend to sign papers allowing hospice to get involved.
At hospice’s suggestion, Maria and I will visit her house in Cambridge Sunday and bring some of her personal effects – her laptop, pillows, photographs – to her room to make it as home-like and familiar as possible.
We will make sure all mail will be read to her if she can’t read it herself. Her address in the hospital is Susan Popper, Room 303 (new room), Saratoga Hospital, 211 Church Street, Saratoga Springs, N.Y., 12866.
Thanks for following this story and for your kind words about these posts. I do appreciate the opportunity to write about life and death; it gives meaning to my work and my life.
I hope to do justice to it.

Jon, your writing has been a comfort to me over the past 27 months I have spent caring for my partner, Pat, who died from advanced pancreatic cancer at age 53 on January 27. My partner also resisted hospice until the very end. She just wanted to keep fighting and insisted on getting chemo long after it was suggested (but not ever directly stated to her by doctors) and wanted to be considered for a clinical trial. She went into septic shock while in the Boston oncologist’s office, discussing a possible clinical trial. We were rushed by ambulance to the ER down the street (not for the first time) and she was hospitalized for a week before being sent home. She died a month later and hospice only entered the picture a few days before she passed, despite my trying and trying to get them involved earlier. She didn’t want to let go and while she was able to die at home, with me by her side, it was not a peaceful passing. She fought until her last breath. Now I am struggling, more than I ever thought possible, as are our children.